A Sustainable Approach to Depression
 In 2018, the EPA worked with eight other mental health-related organisations to produce the policy report “Moving from words to actions”, highlighting the need for a sustainable approach to depression.
In 2018, the EPA worked with eight other mental health-related organisations to produce the policy report “Moving from words to actions”, highlighting the need for a sustainable approach to depression.
Depression is an urgent and growing concern for our societies: the number of people living with depression is rising and is the leading cause of disease burden in high-income countries.
A dedicated website has been launched with resources detailing the 10 key areas of focus needed to improve the lives of people living with depression.
10 Key Factors Identified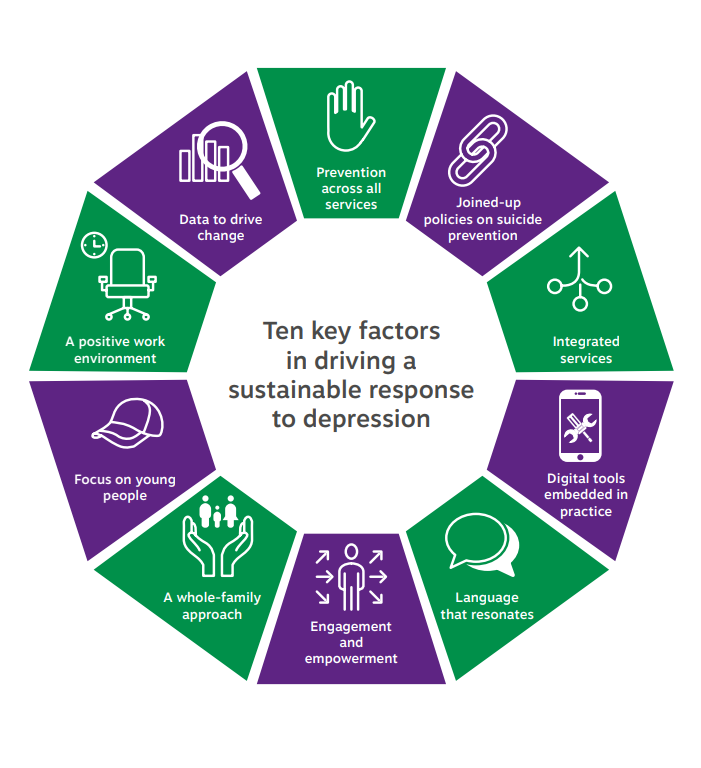
- Incorporate prevention into all services – Prevention is key to responding to the challenge of depression – and a preventive approach should be built into the design of all services. Prevention and early intervention are essential, particularly among younger people and those harder to reach through traditional medical services. Greater clarity about what early intervention means in practice is needed, however, to get more people into appropriate care.
- Create joint government accountability for the prevention of suicide – Prevention of suicide is a key goal in depression care. Suicide can have multiple causes, therefore a cross-sectoral approach to suicide prevention is key. This needs to be reflected in joint government department responsibility and accountability.
- Integrate services to make it easier for people to seek help – The legacy of discrimination around mental health means that people are generally averse to the term ‘mental illness’ and may be disinclined to seek care. Better integration of mental health services within other services may help reach more people. Using a different term, such as ‘wellbeing’, to denote mental health services may also help remove some of the associated stigma.
- Embed digital solutions into practice – Digital health tools can help improve treatment choices for people and encourage them to take greater control of their care. However, these tools can meet resistance from some patients and also from health professionals who may not know how to integrate them into their treatment approach. Better training of health professionals and therapists is needed to facilitate blended care, which combines traditional and digital services.
- Use language that resonates with people – Using language based on people’s experiences of care can be an important therapeutic tool. Terms such as ‘recovery’ are critical to convey a sense of hope and clarify treatment goals. Professionals working with people with depression should be encouraged to use a common language that is easy to understand by everybody and speaks to the experience of those being helped.
- Engage people in their own and others’ recovery – Involving service users and carers in service and policy development will help ensure services work for the people who use them. Services should also draw on the strengths and capabilities of those who have overcome mental health challenges to empower others, for example through peer support.
- Take a whole-family approach to care – Depression can affect the whole family – therefore, treatment should focus on the whole family, not just the person affected. Services that support carers are particularly important to protect their health and wellbeing.
- Empower children and young people to talk about depression – Depression is increasing in young people at an alarming rate. We need to help young people use their own resources and skills to become more resilient and cope better with pressure. Digital tools can break through the isolation of young people battling depression and encourage them to seek help.
- Create a positive work environment for people with depression – Adults spend most of their life in the workplace and depression is one of the leading causes of low productivity. More workplace education programmes are needed to promote a positive workplace culture, help management recognise the signs of depression and support people who are managing depression or returning to work
after taking time off. - Evaluate practices to drive meaningful change – Lack of real-world data is a key gap in depression. We need greater investment in real-world data on the epidemiology of depression, service use and the impact of interventions and services if we are to better understand existing care gaps and implement sustainable change.
To find out more about these recommendations and read the full report, visit the “Words to Actions” website.
